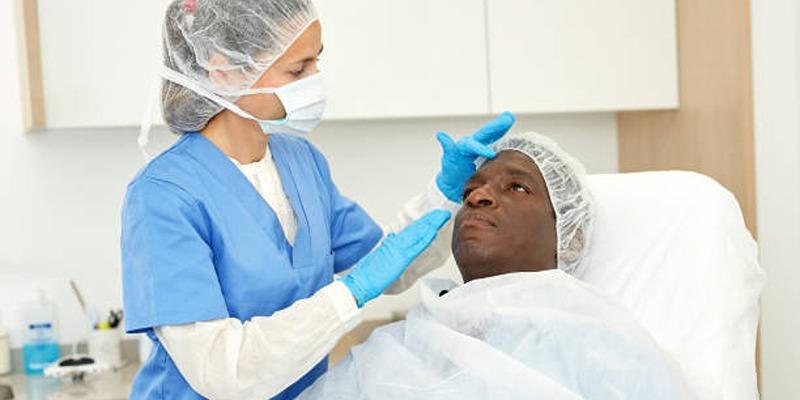
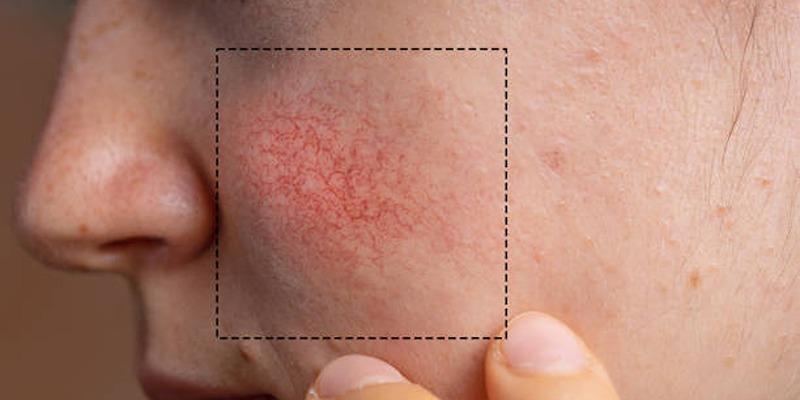
Skin cancer surgery refers to the physical removal of cancerous tissue from the skin, with the primary goal of eliminating malignant cells while preserving as much healthy tissue as possible. Although the concept may seem straightforward, the execution requires careful judgment and precision. Surgeons must balance complete cancer removal with functional and cosmetic considerations, especially when treatment involves visible or sensitive areas.
Unlike therapies that rely on repeated sessions or ongoing monitoring, surgery provides a clear and tangible intervention. For many patients, the idea of removing the cancer directly offers a sense of certainty. At the same time, it is not a one-size-fits-all solution, and its role depends heavily on individual medical factors.
How the Surgery Works
The procedure typically involves removing the visible cancer along with a margin of surrounding tissue. This margin exists to ensure that microscopic cancer cells are not left behind, which helps reduce the likelihood of recurrence. Depending on the size and location of the cancer, the surgery may be brief and performed under local anesthesia, or it may require a more involved approach.
Most skin cancer surgeries are completed in an outpatient setting, allowing patients to return home the same day. During the procedure, surgeons focus on maintaining clean edges and minimizing unnecessary trauma to nearby skin. Afterward, the wound may be closed with stitches or allowed to heal gradually, depending on what best supports recovery. Clear instructions are usually provided to guide wound care and reduce infection risk.
Why Surgery Plays a Key Role
Surgery plays a central role in skin cancer treatment because it addresses the disease at its source. By removing the affected tissue entirely, surgery often provides immediate resolution rather than gradual control. This direct approach can lower uncertainty and reduce the need for extended treatment cycles.
In many cases, surgical removal also allows doctors to examine the tissue more closely after the procedure. This examination helps confirm that the cancer has been fully removed and provides additional information that may guide follow-up care. For patients, this clarity often brings reassurance and a stronger sense of closure.
When Doctors Suggest This Surgery
Doctors do not recommend surgery automatically. The decision depends on several clinical considerations, starting with the type of skin cancer involved. Certain cancers respond particularly well to surgical removal, especially when detected early and confined to a specific area.
The size and depth of the cancer are equally important. Smaller, superficial lesions are often easier to remove completely, while deeper or more extensive growths may still be treated surgically but require careful planning. Location also matters. Areas that experience frequent movement or play an important functional role may need a more tailored surgical approach to support healing and long-term comfort.
Signs Surgery May Be Right for You
Surgery may be an appropriate option when the cancer is localized and has not spread to surrounding tissues. In such cases, removing the lesion can effectively address the problem in a single procedure. Healthy surrounding skin often supports smoother healing and reduces the risk of complications.
Some patients also value the predictability of surgery. Knowing when the treatment will occur and what it aims to accomplish can feel more manageable than ongoing therapies. For individuals who prefer a defined treatment plan with a clear endpoint, surgery often aligns well with those preferences.
Personal Factors to Think About
Beyond medical suitability, personal circumstances influence whether surgery feels like the right choice. Recovery time can vary based on the extent of the procedure and the area treated. While many people resume daily activities within a short period, others may need additional time to rest and heal. Understanding these expectations ahead of time helps reduce stress during recovery.
Appearance after healing is another common concern. Surgeons generally aim to minimize visible scarring, but outcomes can differ depending on individual healing responses. Open discussions about likely cosmetic changes allow patients to make informed decisions and set realistic expectations. Follow-up care also plays a role, as regular check-ins help ensure proper healing and early detection of any future issues.
Questions You Should Ask Your Specialist
Consultations are an opportunity to gain clarity and confidence. Asking about expected outcomes, potential risks, and recovery timelines helps create a clearer picture of what lies ahead. Patients may also want to understand whether alternative treatments exist and why surgery is being recommended over other options.
Clear communication encourages shared decision-making. When patients feel informed rather than rushed, they are better prepared to commit to the treatment plan and follow post-surgical guidance.
Getting Ready for the Surgery
Preparation begins before the procedure itself. Medical teams review health history, medications, and the specific characteristics of the cancer to plan the safest approach. Patients are usually advised on how to prepare on the day of surgery, including guidance on eating, clothing, and skincare.
During the procedure, clinicians typically explain each step as it happens. This transparency helps reduce anxiety and builds trust. After surgery, patients receive instructions on wound care, activity limitations, and signs that may require medical attention. Following these steps closely supports smoother recovery.
Healing and Recovery Process
Healing occurs gradually and often in stages. In the first days after surgery, mild discomfort, swelling, or redness is common and usually improves with proper care. Over time, the skin begins to repair itself, and scars may soften and fade.
Long-term recovery involves more than physical healing. Regular skin examinations become part of ongoing care, helping detect new changes early. These follow-ups support both physical health and peace of mind, reinforcing the value of continued monitoring.
Emotional and Mental Well-Being
A skin cancer diagnosis can bring emotional challenges alongside physical ones. Feelings of anxiety or uncertainty are common, especially before treatment. Many people find that completing surgery provides relief and restores a sense of control.
Support from healthcare professionals, family, or counseling services can help address lingering concerns. Emotional well-being plays an important role in overall recovery, and acknowledging these feelings is part of comprehensive care.
How to Make the Final Decision
Making the final decision involves weighing medical advice against personal comfort and priorities. Reviewing benefits, risks, and remaining concerns can clarify what matters most. Taking time to reflect, while trusting professional guidance, often leads to greater confidence in the chosen path.
Conclusion
Skin cancer surgery is a well-established treatment option that offers clarity and direct intervention for many patients. Understanding how the procedure works, recognizing when it is recommended, and considering personal factors all contribute to informed decision-making. With open communication and thoughtful preparation, surgery can feel less overwhelming and more manageable, supporting both physical recovery and long-term confidence.